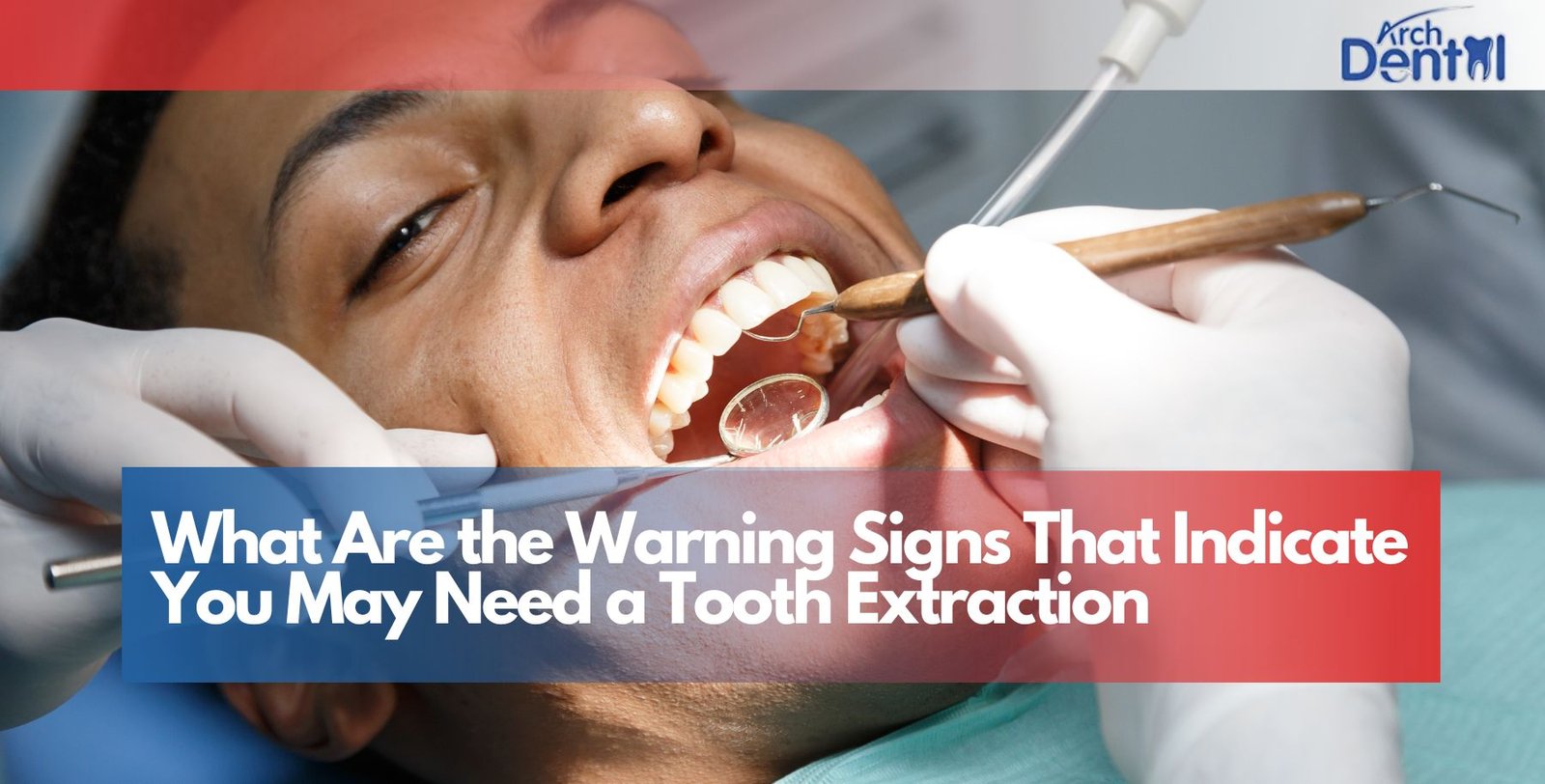
Tooth extraction is never anyone’s first choice in fact, dentists do everything possible to save natural teeth. But sometimes, a tooth becomes so damaged, infected, or misaligned that keeping it can do more harm than good. Recognizing the early warning signs can help you take action before pain and complications get worse.
In this comprehensive guide, we’ll explore the key signs that may indicate you need a tooth extraction, why it becomes necessary, what to expect from the procedure, and how to recover comfortably. By the end, you’ll understand when it’s time to consult a dentist extraction near me and protect your oral health before the problem spreads.
Understanding Tooth Extraction
A tooth extraction is the removal of a tooth from its socket in the jawbone. It’s typically performed when a tooth is too damaged or infected to be repaired through fillings, root canal therapy, or crowns.
Types of Tooth Extractions
There are two primary types:
- Simple extraction: Used for visible teeth. The dentist loosens the tooth and removes it with forceps under local anesthesia.
- Surgical extraction: Needed when a tooth is broken below the gum line or impacted (such as wisdom teeth). The dentist makes a small incision to access and remove it.
Tooth extraction may sound intimidating, but with modern technology, local anesthesia, and sedation options, the procedure is comfortable and straightforward.
Why Tooth Extraction May Be Necessary
Dentists recommend extractions only as a last resort when keeping the tooth could harm your overall oral health.
Common Reasons for Tooth Extraction
- Severe tooth decay or infection
- Impacted wisdom teeth
- Advanced gum disease (periodontitis)
- Overcrowded or misaligned teeth
- Cracked or fractured roots
- Orthodontic treatment needs (to make space)
Knowing the warning signs can help you identify problems early and prevent the need for an emergency extraction.
Warning Sign 1: Persistent Tooth Pain and Sensitivity
Tooth pain is one of the most obvious signs that something is wrong. While occasional sensitivity can happen, constant or sharp pain usually indicates a deeper problem.
When Pain Signals Extraction
If the tooth pain:
- Persists even after taking painkillers
- Worsens when biting or chewing
- Radiates to the jaw or ear
- Is accompanied by swelling or fever
…it could mean that decay or infection has reached the pulp (the inner nerve). In such cases, a root canal may help. But if the infection is too severe or the structure is compromised, extraction may be the only safe option.
What to Do
Don’t ignore tooth pain. Visit your dentist immediately for an examination and X-ray. The longer an infected tooth stays untreated, the higher the risk of the infection spreading to surrounding tissues or bone.
Warning Sign 2: Advanced Tooth Decay
A small cavity can be repaired easily, but when decay spreads deep into the tooth, it weakens the structure and makes restoration difficult.
How Decay Leads to Extraction
Once bacteria reach the pulp, it can cause abscesses — pockets of infection that may lead to severe pain, swelling, or pus discharge. If the tooth can’t be saved through root canal treatment, extraction becomes necessary to protect surrounding teeth and gums.
Preventing Advanced Decay
- Brush twice daily with fluoride toothpaste.
- Floss regularly to remove trapped food particles.
- Limit sugary snacks and drinks.
- Visit your dentist for checkups every six months.
Early detection prevents decay from spreading to the point where extraction is required.
Warning Sign 3: Loose or Shifting Teeth
Adult teeth should never feel loose. If they do, it may indicate periodontal (gum) disease, which affects the tissues that support your teeth.
When Gum Disease Causes Tooth Loss
In advanced stages, bacteria destroy the bone and ligaments holding the tooth in place. Once the support structure weakens, the tooth becomes loose and eventually requires extraction.
Signs of Gum Disease to Watch For
- Bleeding gums when brushing
- Swollen or receding gums
- Persistent bad breath
- Tooth movement or spacing changes
Early gum treatment can prevent tooth loss, but if bone damage is severe, extraction may be unavoidable.
Warning Sign 4: Severe Infection or Dental Abscess
A dental abscess is a pocket of pus that forms due to bacterial infection. It can cause intense pain, swelling, and even fever.
When Infection Becomes Dangerous
If not treated, an abscess can spread to your jawbone, neck, or bloodstream — a serious and potentially life-threatening condition.
Signs You May Have a Dental Abscess
- Throbbing pain in the affected tooth or gum
- Swelling of the face or jaw
- Bad taste or pus discharge
- Fever or swollen lymph nodes
In cases where antibiotics and root canal therapy can’t control the infection, extraction helps prevent further complications.
Warning Sign 5: Impacted Wisdom Teeth
Wisdom teeth (third molars) often cause problems because they don’t have enough space to emerge properly.
How Impacted Teeth Cause Issues
When a wisdom tooth becomes impacted (stuck under the gum or bone), it can push against other teeth, trap bacteria, or form cysts. This can lead to pain, inflammation, and infection.
Symptoms of Impacted Wisdom Teeth
- Jaw pain or stiffness
- Swelling near the back of the mouth
- Difficulty opening your mouth fully
- Gum tenderness or bleeding
Regular dental X-rays can detect impaction early before symptoms worsen.
Warning Sign 6: Cracked or Broken Tooth Beyond Repair
A chipped tooth can often be fixed with bonding or crowns. But if the crack extends below the gum line or into the root, saving it becomes impossible.
When Fractures Require Extraction
Cracks that reach the root canal system allow bacteria to invade the tooth’s interior, leading to infection or structural instability.
Common Causes of Tooth Fractures
- Biting hard foods
- Sports injuries
- Bruxism (teeth grinding)
- Large fillings that weaken the tooth
When restorative options aren’t viable, extraction followed by an implant or bridge is the safest solution.
Warning Sign 7: Overcrowding or Orthodontic Needs
In some cases, teeth may need to be removed as part of an orthodontic treatment plan.
Why Extraction Is Needed Before Braces
Overcrowded teeth can make alignment impossible. Removing one or more teeth allows enough room for the remaining teeth to move into proper position.
When to Consider Extraction for Alignment
- Teeth overlap or twist significantly.
- There’s not enough space for all teeth.
- Your bite alignment affects speech or chewing.
Extraction in these cases is preventive it ensures successful orthodontic results.
Warning Sign 8: Chronic Gum Pain and Swelling
Constant gum inflammation can mean that bacteria have penetrated deep into your gum tissues or bone.
Gum Infections and Extraction
In advanced gum disease, teeth become unstable due to bone loss. When teeth can’t be saved with deep cleaning or surgery, extraction prevents further spread and discomfort.
How to Protect Your Gums
- Use an antibacterial mouthwash.
- Quit smoking — it slows gum healing.
- Schedule professional cleanings twice a year.
Warning Sign 9: Tooth Mobility After Trauma
A strong impact from sports or an accident can loosen or dislodge a tooth.
When Trauma Leads to Extraction
If the tooth root or surrounding bone is fractured, it might not be possible to stabilize it. In such cases, removal may be necessary to prevent infection or alignment issues.
Prompt treatment after trauma is crucial early intervention can sometimes save the tooth.
Warning Sign 10: Cysts or Tumors Around Teeth
Sometimes, cysts or benign growths form near the roots of teeth. While not always painful, they can damage bone and nerves if untreated.
When Extractions Are Necessary
If a cyst forms around an impacted tooth or infected root, extraction is often required to remove both the tooth and the lesion safely.
Your dentist may recommend imaging tests to evaluate the extent of the condition before proceeding with surgery.
What Happens During a Tooth Extraction
Knowing what to expect can help you feel more comfortable before your procedure.
Step 1: Consultation and X-Rays
Your dentist evaluates your tooth, surrounding bone, and gums using digital X-rays.
Step 2: Anesthesia
Local anesthesia numbs the area. Sedation may be used for anxious patients or complex extractions.
Step 3: Extraction
For a simple extraction, the tooth is loosened and gently removed. For surgical extractions, a small incision is made to access the tooth.
Step 4: Post-Extraction Care
After removal, your dentist places gauze to stop bleeding and provides care instructions for healing.
Most patients recover within 7–10 days and can return to normal activities soon after.
What to Expect After a Tooth Extraction
Healing after extraction is generally smooth with proper care.
Aftercare Tips
- Bite gently on gauze to control bleeding.
- Apply an ice pack to reduce swelling.
- Avoid smoking, spitting, or using straws for 48 hours.
- Eat soft foods and stay hydrated.
- Brush gently around the extraction site.
If pain, swelling, or bleeding persists beyond three days, contact your dentist immediately.
How to Replace an Extracted Tooth
Leaving a gap after extraction can lead to bone loss and shifting of nearby teeth. Fortunately, there are several options to restore your smile.
Dental Implants
A titanium post replaces the tooth root and supports a crown that looks and feels natural.
Dental Bridges
A prosthetic tooth anchored to surrounding teeth. Ideal for single-tooth replacement.
Dentures
Partial or full removable replacements for multiple missing teeth.
Replacing extracted teeth promptly preserves your bite and bone health long-term.
Prevention: How to Avoid Tooth Extraction
Tooth extraction is preventable in most cases through consistent oral care.
Daily Prevention Routine
- Brush twice daily with fluoride toothpaste.
- Floss daily to remove food particles.
- Avoid excessive sugar and acidic foods.
- Schedule routine dental exams every six months.
Early intervention is key — catching decay, infection, or gum issues early can save your natural teeth.
When to See a Dentist for Possible Extraction
If you experience persistent pain, swelling, bleeding gums, or a loose tooth, don’t wait. These symptoms may indicate an infection or structural issue that needs professional attention.
Prompt diagnosis ensures that treatment options remain available before extraction becomes necessary.
Conclusion
Tooth extraction isn’t just about removing a damaged tooth — it’s about protecting your overall health and preventing further complications. Whether it’s due to severe decay, infection, or crowding, your dentist will only recommend extraction when it’s truly the best solution.
If you notice warning signs such as persistent pain, swelling, or tooth mobility, schedule a consultation with your dentist Northampton to assess your condition and explore treatment options. Timely care can often save your tooth, but when extraction is necessary, it ensures a healthier, pain-free future for your smile.
FAQs
Can tooth extraction affect my speech or chewing ability in the long term?
Yes, temporarily. After extraction, you may notice mild changes in speech or chewing until your mouth adjusts. Replacing the extracted tooth with a dental implant, bridge, or denture restores full function and prevents bite issues.
Can a cracked or fractured tooth always be saved, or will it need extraction?
Not always. If the crack extends into the root or below the gum line, extraction is often required to prevent infection. However, minor cracks can often be repaired with crowns or bonding if detected early.
How does tooth extraction affect adjacent teeth?
If a gap is left unfilled, nearby teeth can drift or tilt into the empty space, causing misalignment and bite problems. Replacing the missing tooth promptly helps maintain dental structure and prevents uneven wear.
What happens if I delay a needed tooth extraction?
Delaying extraction can lead to infection, bone loss, abscess formation, and severe pain. In some cases, the infection can spread to other parts of the body. Early treatment prevents complications and speeds recovery.
Is tooth extraction safe for people with medical conditions?
Yes, with proper planning. Patients with diabetes, heart disease, or other conditions can safely undergo extractions under a dentist’s supervision. Your dentist will review your medical history and coordinate care with your physician if necessary.